
Multi-Omics in Rare Disease Studies: Case Examples
Integrating genomics, transcriptomics, proteomics and metabolomics improves rare disease diagnosis and uncovers mechanisms guiding treatment.

Integrating genomics, transcriptomics, proteomics and metabolomics improves rare disease diagnosis and uncovers mechanisms guiding treatment.

Explains how FDA expanded access gives investigational drugs to rare disease patients, outcomes, barriers and policy solutions.

Clear guide to FDA orphan drug designation: eligibility, 90-day review, tax credits, fee waivers, and 7-year market exclusivity.

Comprehensive roundup of 10 tools that link genetic variants and clinical phenotypes to speed rare disease diagnosis and personalize care.

Comprehensive roundup of 10 tools that link genetic variants and clinical phenotypes to speed rare disease diagnosis and personalize care.

Six modern treatments for rare genetic disorders: small molecules, ASOs, gene therapy, genome editing, combos, and AI-personalized drugs.

How patient-derived iPSCs, organoids, and PDX models improve drug discovery, personalized therapies, and their limits.

Gene editing, ASOs and patient‑derived iPSCs are reshaping rare disease care, enabling faster, tailored treatments and adaptive regulatory pathways.

When a family comes to RareLabs, one of the first things we explain is this: we don't put all our eggs in one basket. Rare disease research is inherently uncertain — no one can predict in advance which approach will yield the most promising results for any given condition.

One of the most powerful tools in modern rare disease research is something that would have sounded like science fiction just twenty years ago: taking a patient's own cells and transforming them into a living, testable model of their disease in the laboratory. This technology — known as induced

A rare disease is any condition that affects fewer than 200,000 people in the United States. But the word "rare" can be deeply misleading. There are over 10,000 known rare diseases worldwide, and collectively they affect an estimated 400 million people globally — roughly 30 million in

Seven-step checklist to choose genetic therapies, use patient-derived models, confirm safety, and plan translation for rare diseases.

Seven-step checklist to choose genetic therapies, use patient-derived models, confirm safety, and plan translation for rare diseases.
Families facing rare genetic diseases fund research, build registries, use iPSCs and custom therapies when no approved treatment exists.
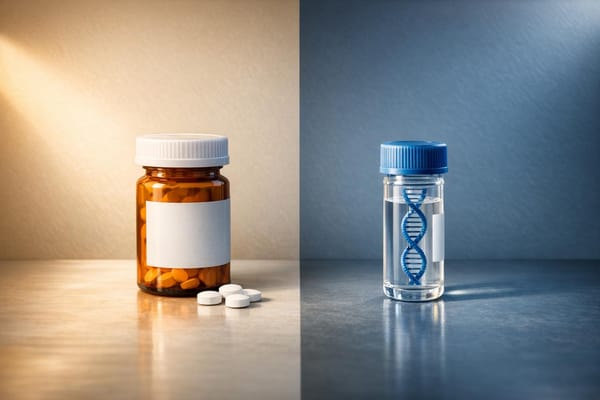
Small molecules give accessible symptom control; gene replacement targets genetic causes but brings higher cost and delivery risks.

Questions to ask before starting rare disease treatment—confirm genetic diagnosis, compare therapies, weigh risks and costs, and plan long-term follow-up.

Compare gene therapy and antisense oligonucleotides: DNA vs RNA targets, durable vs reversible effects, delivery methods, and best-use cases for rare genetic diseases.

A 5-step plan to pursue treatment for rare genetic diseases: confirm diagnosis, join advocacy groups, research repurposed drugs, explore personalized therapies, and prepare for trials.

Integrated omics plus AI improve rare-disease diagnosis and target ID, enabling personalized, combination therapies tested in patient-derived models.